I was supposed to be charge nurse yesterday. But because staffing remained incredibly tight, and we had some extraordinarily sick patients in our unit right now (four on CVVH, a nurse-driven specialized form of slow dialysis; and one little baby on ECMO, the ultimate heart-lung machine for the sickest of patients), one of our wonderfully supportive supervisors came in to fill the charge nurse position and I became Resource Nurse, the nurse who goes around the unit the entire day to help with emergencies, procedures, especially busy patients and traveling to places like CT scans and MRIs.
I barely sat down to get a morning report at 0700 when the emergency pager went off. The medical-surgical floor upstairs was calling for the Rapid Response Team to come assess a patient in respiratory distress. I got the skinny version of the update on the busiest or sickest patients in the unit, and then joined our Fellow to see this patient upstairs, hoping he wouldn’t need a highly coveted ICU bed, but sure enough, he did. I returned to the unit and brainstormed with the charge nurse to see how we might move patients and nurses around to make space.
It was only 0750 when I got another call from the nurse taking care of the ECMO patient. There were neurological changes that were concerning, and she’d need to take this patient – connected to a ventilator with a breathing tube, to a machine delivering Nitric Oxide, to multiple IV pumps, and to the ECMO machine acting as the patient’s heart – three floors downstairs for a STAT CT scan. This trip required two nurses, two ECMO specialists, two respiratory therapists, and one attending physician to ensure a safe trip and scan.
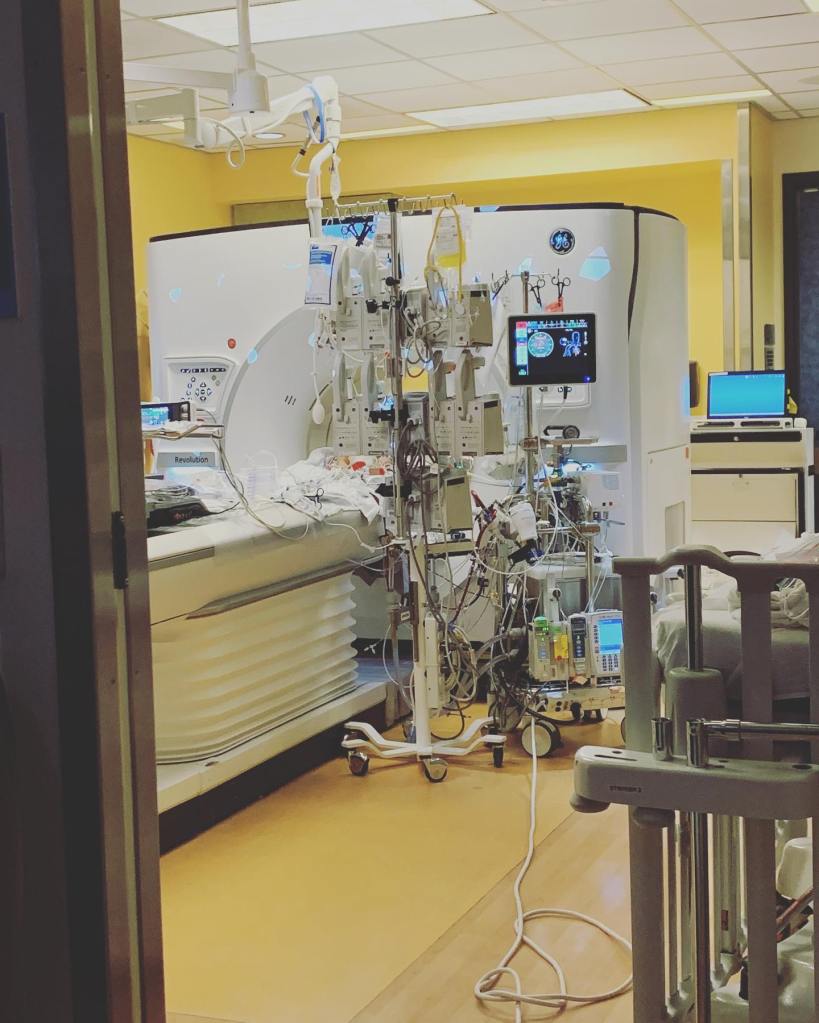
Unfortunately, while the trip itself went fairly smoothly, the scan only confirmed what we feared. The baby had suffered irrevocable neurological damage.
My day started already running off to an emergency, and then to a critically important stat CT scan with a very involved patient. The middle of my day involved going to room after room helping colleagues manage their dialysis circuits, suctioning their patients struggling to keep oxygen levels up, and relieving them for much-needed breaks. My day ended with providing sobering post-mortem care on the baby we had transported to CT scan that morning.
This is a day in the life of a PICU nurse in December 2022.
Below is the reflection I wrote from the day, after I got home around 8:20pm.
***
Why do I talk so much about nursing? It’s not my core identity. But the role of pediatric ICU nurse shapes my core more than probably any other role in my life.
From the start of a singular 12 hr shift, I am thrust past all the BS and pettiness of the world, all my personal dumb self-absorption, all my ingratitude and entitled assumptions.
I get to see how a short-staffed team of people will mobilize and rally to get one pivotal CT scan for one very sick baby.
I get to see the very best of people meet the very worst that life throws at one singular family… and the next, and the next room in a unit of very, very sad stories.
I get to see how grace finds us caregivers when we feel weak and weary and threadbare, and still we weave together to knit comfort for those who have otherwise been stripped naked of all consolation.
I get to see how love endures all things and surely never ends, even after all the life support is peeled away and I am quietly shrouding a tiny person while his family whispers his name and promises he will live forever in their hearts.
I get to be in the most sacred of spaces and as indescribably hard as this job is right now,
it is still such a privilege to be a nurse.
Pingback: An ICU Nurse’s Complicated Relationship with the Turn of the New Year | The Heart of Nursing